Epidermal vs Dermal Hyperpigmentation
Epidermal vs Dermal Hyperpigmentation, known by many South Africans as Chubaba, is not a uniform condition, its behavior is dictated entirely by the depth at which the pigment sits. In my experience treating South African skin types, the most common oversight is failing to distinguish between discoloration in the epidermis (the skin’s surface layer) and deposits held within the dermis.
This distinction is critical because it directly determines the “stubbornness” of your hyperpigmentation. Our skin produces melanin as a result of a complex biological process called Melanogenesis. This process takes place inside specialized cells called melanocytes, which are located at the basal layer, the very bottom foundation of the epidermis.
According to clinical studies on melanogenesis, treating dermal pigment with an epidermal-only approach is the leading cause of treatment failure. Understanding the skin architecture is the first step to choosing the correct routine and setting realistic expectations for your recovery timeline. That said, you don’t need to study like a doctor. You simply need to understand your skin just enough so that everything finally makes sense and you know exactly what you are dealing with.
Table of Contents
The Three-Layer Map of Pigment
The Three-Layer Map of Pigment
To understand your skin, think of it in three distinct sections. Each layer dictates how your pigmentation looks and, more importantly, how we must treat it.
1. Understanding Epidermal Hyperpigmentation: The Surface Layer
This is the surface you see. It is your skin’s “protective shield”. Its main job is to keep the good things in (like water) and the bad things out (like bacteria), and it is constantly renewing itself. That full cycle takes about 28 days.
This is where common sun spots and post-acne marks live. Because this layer is in a state of constant renewal, shedding old cells and replacing them with new ones, hyperpigmentation at this level is the most responsive to treatment. When you use the correct topical formulas, you are essentially accelerating the removal of these “stained” cells as the skin naturally refreshes itself.
2. The Foundation Layer (The Basal Junction)
This layer sits at the very bottom of your top skin. It is the most important part of the story because this is where your skin’s color is actually created. This layer is also known as the Basal Membrane (or the Dermal-Epidermal Junction). It is like the “security floor” that separates your top skin from the deep layer.
This is where melanogenesis happens. This is where your melanocytes live and breathe. If you don’t address this middle layer, you are only treating the symptoms on the surface without stopping the origin point from overproducing the pigment that creates your hyperpigmentation.
3. The Deep Layer: Understanding the Dermis and Dermal Pigmentation
This is the thick, structural foundation of your skin that sits beneath the middle layer. It contains your collagen, elastin, and blood vessels.
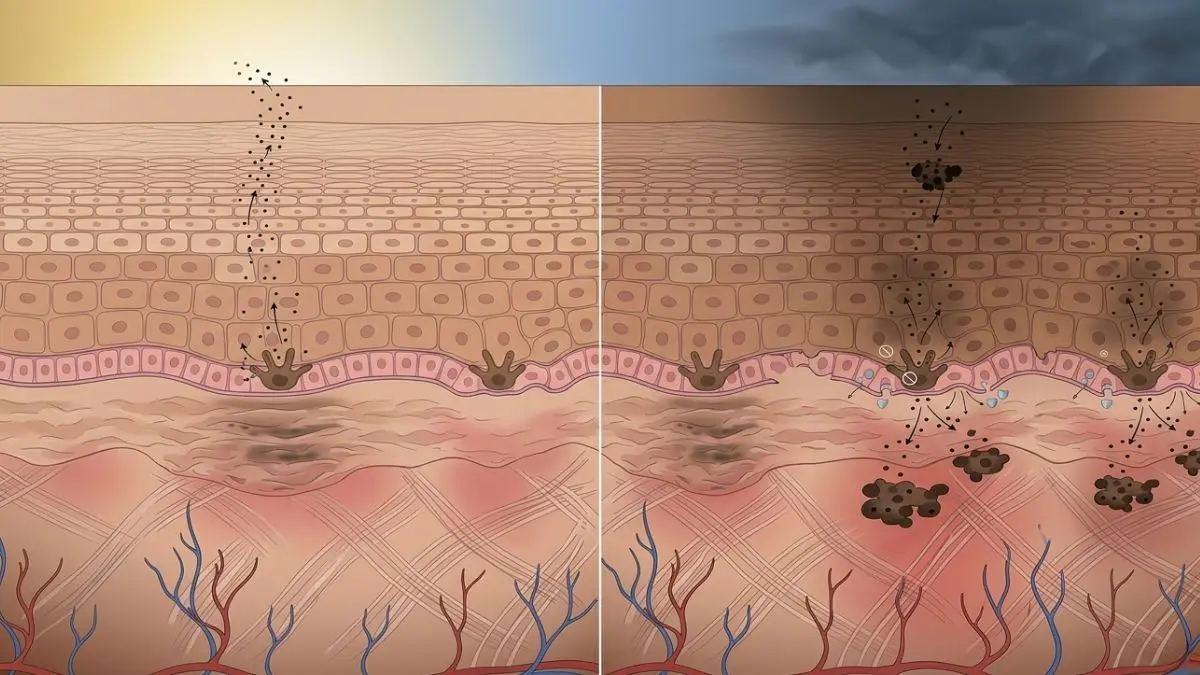
Normally, pigment is created in the middle layer and is transferred upward to the top layer (the epidermis) to eventually be shed away. However, sometimes the pigment can drive downwards instead of upwards. It travels downwards when there is severe inflammation or when the cells in the middle layer become “leaky” or damaged. When the pigment reaches this deep layer, it is called dermal pigmentation.
Epidermal vs Dermal Hyperpigmentation- The Biological Journey of Pigment
Melanin production begins in the melanocytes, which sit at the bottom (Basal) layer of the epidermis. When your skin is triggered, by UV exposure, inflammation, or injury, these cells activate an enzyme called tyrosinase. This enzyme converts the amino acid tyrosine into melanin, the pigment responsible for skin color.
Once produced, the melanin is packaged into tiny structures called melanosomes. These melanosomes are then transferred from the melanocytes into the surrounding cells called keratinocytes. These are the main cells that make up your skin.
From here, the process follows a natural upward pathway. As part of your skin’s normal renewal cycle, these keratinocytes slowly move from the bottom layer up through the epidermis. As they move, they carry the pigment with them toward the surface. Over approximately 28 days, these cells reach the top layer and are eventually shed off. This is how pigmentation is naturally removed from the skin.
The “Leaky” Membrane Reality
However, this system only works properly when the skin is healthy. When there is significant inflammation or damage, the bottom (basal layer) can become compromised.
This isn’t just a theory; it is a clinical reality. A landmark study published in the Journal of Dermatology (available on PubMed) found that 95.5% of melasma lesions showed actual physical damage to the basal membrane. This damage is what creates the ‘pathway’ for pigment to fall into the dermis, where it becomes trapped.
Instead of melanin moving upward, some of it leaks downward into the dermis. Once pigment enters this deeper layer, it is no longer part of the normal shedding cycle, which is why dermal pigmentation becomes much more persistent and difficult to treat. Because it is “trapped” below the shedding surface, it cannot be scrubbed away or simply lightened with standard surface exfoliants.
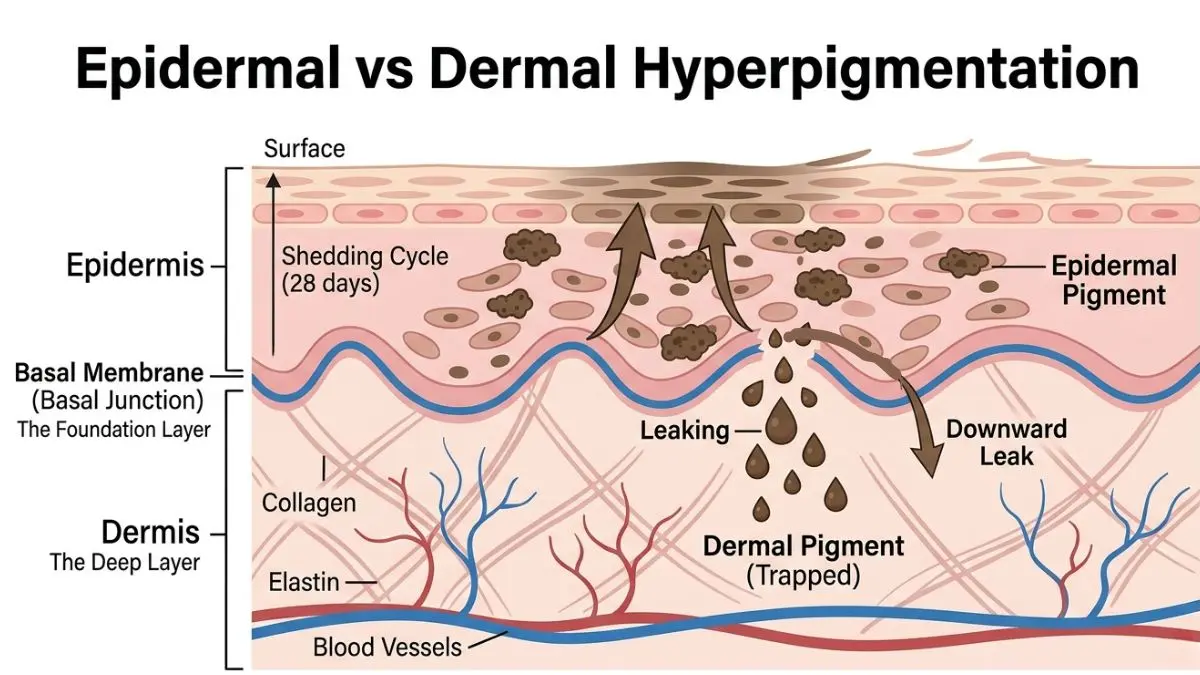
Caption: Epidermal pigment rises naturally with the 28-day shedding cycle, while dermal pigment occurs when melanin “leaks” through the basal membrane and becomes trapped in the deep layer.
The 6-Path Strategy for Epidermal vs Dermal Hyperpigmentation
To address pigment that has “leaked” into the dermis versus pigment sitting on the surface, we have to look at the six biological “checkpoints” in the skin:
1. Tyrosinase Inhibition: This is the “Stop” signal. We must inhibit the enzyme Tyrosinase at the Basal Layer to prevent new melanin from being synthesized.
- The Solution: Our Melanin Breaker targets this factory directly with 4-Butylresorcinol and SymWhite 377.
2. Melanosome Transfer: Even if pigment is made, it has to be “delivered” to your skin cells. We use actives to interrupt this delivery truck so the pigment stays away from the surface.
- The Solution: This is a core function of the multi-active approach in the Melanin Breaker.
3. Antioxidant Defense: Free radicals from the South African sun act as “fuel” for your melanocytes. We must neutralize this fuel to keep the factory quiet.
- The Solution: The Tetrahexyldecyl Ascorbate (Lipid-Soluble Vitamin C) in our Melanin Breaker provides deep-reaching antioxidant protection that doesn’t wash off.
4. Anti-Inflammatory Stabilization: Since dermal pigment is often caused by a “leaky” basal membrane due to inflammation, we must calm the skin’s “internal heat” to stop the downward leak.
- The Solution: Our Barrier Repair Cream is designed to stabilize the skin and lower the inflammatory “heat” that triggers the leak.
5. Desquamation (Shedding): For the epidermal (surface) pigment, we must support the 28-day shedding cycle to ensure stained cells are moved off the skin’s surface.
- The Solution: While our Pigmentation Exfoliant (Acids) unglues the dead cells on the surface, our Retinoid Firming Cream works from the inside out to speed up the entire 28-day cycle.
6. Structural Barrier Repair: We must seal the skin. A compromised barrier allows external triggers to reach the deeper layers, causing the very inflammation that drives pigment downward into the dermis.
- The Solution: Our Barrier Repair Cream acts as the “Structural Seal”. It calms the internal heat and reinforces the junction between the top and deep skin. This stops the “Downward Leak,” ensuring pigment moves UP to be cleared, rather than DOWN to be trapped.
The Real Truth About Epidermal vs Dermal Hyperpigmentation
The “Real Truth” is that you cannot treat Dermal and Epidermal Hyperpigmentation the same way. One is moving up (and can be cleared), while the other is trapped down (and must be stabilized).
If you treat your skin like a “stain” to be scrubbed, you will only damage the Basal Junction further, leading to more leakage and more stubborn “Chubaba”. Understanding where your pigment lives is the only way to choose a routine that actually works.
Investigate Further: Download: Why is my Melasma or Dark Spots Getting Darker?
Read: Melasma and Hyperpigmentation: Causes, Treatments, and How to Fade Dark Patches
Common Questions: Epidermal vs Dermal Hyperpigmentation
While a clinical skin analysis is best, epidermal pigment usually appears as well-defined, brown patches that may darken after sun exposure. In contrast, dermal hyperpigmentation often has a fuzzy, bluish-gray or "ashy" cast and sits much deeper in the skin's architecture, making it appear more "shadowy" than a surface stain.
Because dermal pigment is "trapped" beneath the Basal Membrane, surface exfoliation cannot reach it. Aggressive scrubbing actually triggers more inflammation, which can further damage the membrane and cause even more pigment to leak downward, making your hyperpigmentation worse.
No. The 28-day shedding cycle only moves cells through the Epidermis. Once pigment leaks into the Dermis, it is no longer part of that natural "conveyor belt" and will not be shed away, which is why dermal staining requires stabilized, deep-reaching tyrosinase inhibitors.
Yes. This is the "Leaky Membrane" reality. Severe or chronic inflammation can compromise the junction between your top and deep skin layers. When this "security floor" fails, melanin that should have moved up to be shed instead falls down into the dermis, turning a simple surface spot into stubborn dermal hyperpigmentation.
The most critical step is Structural Barrier Repair. By sealing the skin and calming the "internal heat" of inflammation, you stop the downward leak at the source. Once the barrier is stabilized, you can then focus on inhibiting the pigment factory and clearing the surface stains.
About Sharika Regchand
Sharika Regchand is a veteran investigative journalist and researcher with over two decades of experience in high-stakes legal and investigative reporting. Now a skincare author and formulator, she applies that same investigative rigor to the science of cosmetic chemistry, conducting in-depth interviews with skincare users for research purposes, analyzing real-world outcomes, and deconstructing complex studies to uncover the definitive truth behind ingredient efficacy, formulation stability, and skin safety.
View all posts by Sharika Regchand